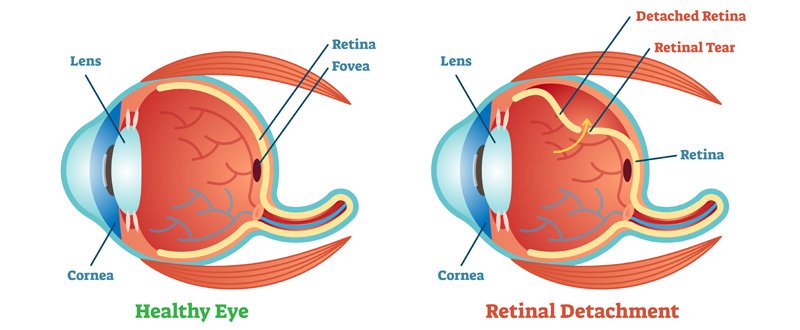
A retinal detachment occurs when the retina is pulled away from its normal position in the back of the eye. The retina is the light-sensitive layer of tissue that lines the inside of the eye and sends visual messages through the optic nerve to the brain. Retinal detachment can cause permanent vision loss if not treated in time.
What are the types of Retinal Detachment?
There are three types of RD:
- Rhegmatogenous Retinal Detachment: A rhegmatogenous retinal detachment occurs due to a hole or breaks in the retina that allows fluid to pass into the space between the retina and other layers of the eye.
- Exudative or Secondary Retinal Detachment: An exudative retinal detachment occurs due to inflammation that results in fluid accumulating underneath the retina without the presence of a hole or break.
- Tractional Retinal Detachment: A traction retinal detachment occurs when fibrovascular tissue on the surface of retina pulls the retina from the underlying tissues as seen in diabetic retinopathy cases.
What are its symptoms?
- Flashes of Light (Photopsia): mostly experienced in the temporal (outside away from the nose) part of the vision
- Floaters: black cobweb-like spots moving in front of the eye
- A curtain-like shadow coming in the field of vision
- Sudden Vision Loss when macula is detached
Who is at risk for Retinal Detachment?
A retinal detachment can occur at any age, but it is more common in people over the age of 40. Common risk factors for developing RD are:
- High Myopia, especially more than 5 Dioptre, after cataract surgery
- Retinal detachment in the other eye
- Family history of RD
- Presence of other eye diseases such as retinoschisis, degenerative myopia, or lattice degeneration
- Following an eye injury
What are the treatment options?
Retinal hole or breaks are treated with laser photocoagulation or cryopexy (a freeze treatment) as the outdoor procedure. During laser treatment, dot-like burns are placed around the hole to “weld” the retina. In Cryopexy the area around the hole is frozen, and it helps reattach the retina. Retinal detachments are treated with surgery viz scleral buckling and complex vitreoretinal surgery involving the use of Silicon oil or gases.
- In scleral bucking, a silicone band is placed anchored with stitches around the eyeball to gently push the wall of the eye against the detached retina.
- In vitrectomy, the surgeon makes tiny incisions in the sclera (white portion of the eye). Vitrectomy instruments are placed inside the eye to take out the vitreous gel, and it is replaced with silicone oil or gases to push the retina in place. Laser or cryopexy is done around the breaks to seal it.
With modern vitreoretinal instrumentation, around 90 percent of cases with a retinal detachment can be successfully treated. Visual results are good if the retinal detachment is repaired before the macula (the centre region of the retina responsible for fine, detailed vision) detaches. It is important to contact your retina surgeon in time when you notice any flashes or floaters or a curtain in the field of the vision.