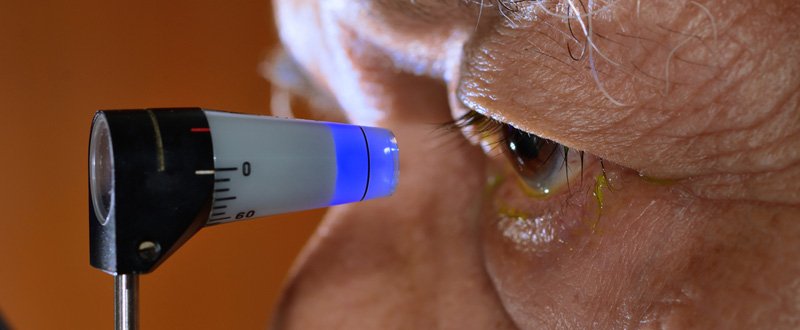
Glaucoma is the most serious eyesight threatening condition. It usually manifests as a painless, gradual loss of vision. The lost vision can never be recovered. However, medical or surgical treatment can prevent or retard further loss of vision.
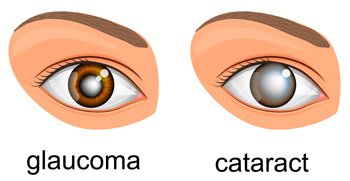
Do Not Confuse Glaucoma with a Cataract
Our eyes contain a clear fluid called aqueous humor, which is continuously produced in the eye to bath and nourish the structures inside it. The fluid normally drains out of the eye through drainage canals in a fine meshwork located around the edge of the iris (the colored part of the eye that surrounds the pupil). In people with glaucoma, the fluid fails to drain due to some defect and thus increases the pressure inside the eyes called raised Intraocular Pressure (IOP) (or Tension).
Who is at a Risk for Glaucoma?
Anyone can develop glaucoma. Some people are at higher risk than others. They include:
- Everyone over the age of 40 yrs.
- People with family history of glaucoma.
- Diabetics
- People with near sightedness (Myopia) for open angle type and far sightedness (hyperopia) for close angle type
- People with Hypertension
- People with Migraines
Common Symptoms of Glaucoma
In most cases of glaucoma, the patient is not aware of the gradual loss of sight until vision is significantly impaired. However, if glaucoma progresses without adequate treatment, the following symptoms may occur in some individuals:
- Pain around the eyes when coming out from darkness (e.g., as soon as the person comes out of a cinema hall)
- Colored halo rings seen around light bulbs especially in the mornings and nights
- Frequent change of reading glasses, headaches, pain, and redness of the eyes
- Reduced vision in dim illumination and during nights
- Gradual decrease of side vision with the progression of glaucoma
Types of Glaucoma
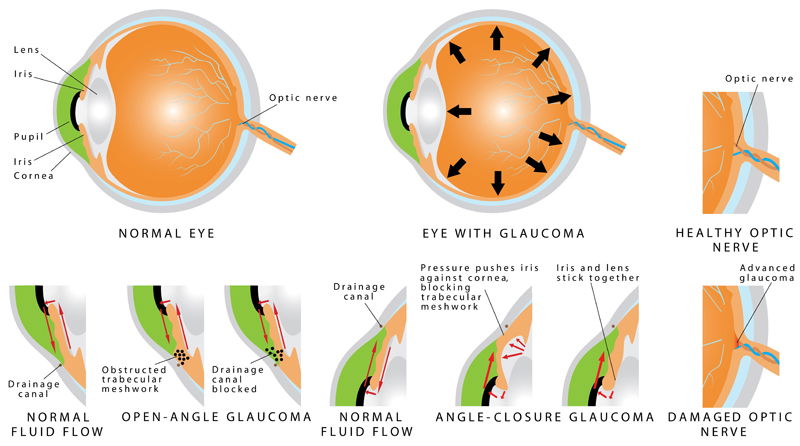
Open-Angle Glaucoma
It happens when the eye’s drainage canals become clogged over time. The inner eye pressure (also called intraocular pressure or IOP) rises because the correct amount of fluid can’t drain out of the eye. With open-angle glaucoma, the entrances to the drainage canals are clear and open. The clogging problem occurs further inside the drainage canals, similar to a clogged pipe below the drain in a sink. Most people have no symptoms and no early warning signs. If open-angle glaucoma is not diagnosed and treated, it can cause a gradual loss of vision. This type of glaucoma develops slowly and sometimes without noticeable sight loss for many years. It usually responds well to medication, especially if caught early and treated. This form of glaucoma is more common in Caucasians than others.
Angle-Closure Glaucoma
This type of glaucoma is also known as acute glaucoma or narrow-angle glaucoma. It is more common in Asians and is very different from open-angle glaucoma in which the eye pressure usually rises very quickly. It happens when the entrance to the drainage canals is very narrow or covered over, like a sink with something covering the drain. Symptoms of angle closure glaucoma may include headaches, eye pain, nausea, rainbows around lights at night, and very blurred vision.
Low-Tension or Normal-Tension Glaucoma
In this type of glaucoma, the optic nerve is damaged even though intraocular pressure (IOP) is not very high. Lowering eye pressure by at least 30 percent through medicines slows the disease in some people. A comprehensive medical history is essential in identifying other potential risk factors, such as low blood pressure, that contribute to low-tension glaucoma. If no risk factors are identified, the treatment options for low-tension glaucoma are the same as for open-angle glaucoma.
Congenital Glaucoma
Children are born with a defect in the angle of the eye that slows the normal drainage of fluid. These children usually have visible symptoms, such as cloudy eyes, sensitivity to light, and excessive tearing. Conventional surgery typically is the suggested treatment, because medicines may have unknown effects in infants and be difficult to administer. The operation is safe and effective. If surgery is done promptly, these children usually have an excellent chance of having good vision.
Secondary Glaucoma Types
These can develop as complications of other medical conditions. These types of glaucoma are sometimes associated with eye surgery or advanced cataracts, eye injuries, certain eye tumors, or uveitis (eye inflammation). Pigmentary glaucoma occurs when pigment from the iris flakes off and blocks the meshwork, slowing fluid drainage. A severe form, called neovascular glaucoma, is linked to diabetes. Corticosteroid drugs used to treat eye inflammations, and other diseases can trigger glaucoma in some people. Treatment includes medicines, laser surgery, or conventional surgery.
Standard Investigation for Glaucoma
Early detection, through regular and complete eye exams, is the key to protecting your vision from damage caused by glaucoma. Following are the ways through which you can get your eyes examined for Glaucoma:
Applanation Tonometry
The tonometry test measures the inner pressure of the eye. Usually drops are used to numb the eye. Then the doctor or technician will use a special device that measures the eye’s pressure.
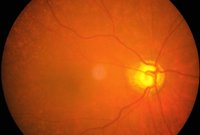
Ophthalmoscopy
Ophthalmoscopy is used to investigate the inside of the eye, especially the optic nerve. In a darkened room, the doctor will magnify your eye by using an ophthalmoscope (an instrument with a small light on the end). It helps the doctor look at the shape and color of the optic nerve.
Perimetry
Perimetry is a procedure where the patient wears a patch over one eye and looks straight ahead at a bowl-shaped white area. At the same time, the computer presents lights in fixed locations around the bowl. The patient indicates each time he or she sees the light, which is why perimetry can provide a map of the visual fields. The type of vision loss associated with glaucoma is relatively specific, and perimetry can detect the typical visual-field defects of glaucoma disorder. The perimetry test is also called a visual field test.

Gonioscopy
Gonioscopy is used to detect which type of glaucoma you have. Once the surface of the eye has been numbed with eye drops, your eye specialist will place a special contact lens on your eye. This lens will allow your eye specialist to look at the eye’s drainage system and check if the angle where the iris meets the cornea is open or closed.
Newer Diagnostics for Glaucoma
Retinal Nerve Fibre Analysis/OCT
Retinal Nerve Fibre Analysis/OCT Nerve fiber analysis is a newer method of glaucoma testing in which the thickness of the nerve fiber layer is measured. Thinner areas may indicate damage caused by glaucoma. This test is especially suitable for patients who may be considered to be a glaucoma suspect and also to indicate if a person’s glaucoma is progressively becoming worse. The OCT instrument utilizes a technique called optical coherence tomography which creates images by use of special beams of light. The OCT machine can produce a contour map of the optic nerve, optic cup and measure the retinal nerve fiber thickness. Over time this machine can detect loss of optic nerve fibers.
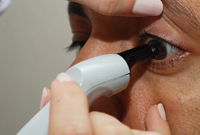
Pachymetry
Pachymetry is the method of measuring the thickness of the cornea. Corneal thickness is critical because it can mask an accurate reading of eye pressure, causing doctors to treat you for a condition that may not really exist or to treat you unnecessarily when are normal. Actual IOP may be underestimated in patients with thinner CCT and overestimated in patients with thicker CCT. Pachymetry is a simple, quick, painless test With this measurement; your doctor can better understand your IOP reading, and develop a treatment plan that is right for your condition. The procedure takes only about a minute to measure both eyes.
Laser Peripheral Iridotomy – A Treatment for Acute Angle Closure Glaucoma
Patients with narrow, occlude-able angles or who have an attack of acute angle closure glaucoma are treated with laser peripheral iridotomy (LPI).
Laser peripheral iridotomy involves creating a tiny opening in the peripheral iris, allowing aqueous fluid to flow from behind the iris directly to the anterior chamber of the eye. It typically results in resolution of the forwardly bowed iris and, thereby, an opening up of the angle of the eye. The narrow or closed angle thus becomes an open angle. Before the advent of the laser, surgery was necessary to create this bypass (surgical iridectomy).
The laser peripheral iridotomy procedure is completed in the office. Before the procedure, the pupil is often constricted with an eye drop medication known as Pilocarpine. Usually, a lens is placed on the eye (after topical anesthetic drops are applied) to control the laser beam better. The entire procedure takes only a few minutes. The lens is then removed from the eye, and vision will quickly return to normal. After the procedure, we may recommend anti-inflammatory eye drops for the next few days, and a post-operative visit will be scheduled.
Laser FAQs
Often, patients having a laser PI do not have glaucoma. This procedure is being done prophylactically to prevent the development of angle closure glaucoma. In the cases where there is pre-existing chronic open angle glaucoma or attacks of acute angle closure glaucoma, the treatment should prevent further damage to the nerve.
The surface of the eye is numbed by topical anesthetics for this procedure, but the iris is not; therefore, when the laser beam hits the iris to create the peripheral iridotomy, mild discomfort may occur. In general, only a few brief episodes of slight discomfort are associated with this procedure. Also, there is no discomfort postoperatively in the great majority of cases.
A laser peripheral iridotomy is an extraordinarily safe procedure. Complications, fortunately, are very rare. Potential complications include bleeding in the eye, inflammation in the eye, and transient pressure elevations. Therefore, we recommend treatment with an anti-inflammatory drop following the procedure.
Glaucoma Treatment in Delhi at Eye7 Chaudhary Eye Centre
Glaucoma is a chronic (long-lasting) progressive condition. Any vision loss that had occurred, before glaucoma was diagnosed, cannot be reversed. Glaucoma treatments at Eye7 Chaudhary Eye Centre include medicines, laser trabeculoplasty, conventional surgery, or a combination of any of these. While these treatments may save remaining vision, they do not improve sight already lost from glaucoma.
- Medicines: Medicines, in the form of eye drops or pills, are the most common early treatment for glaucoma. Some medicines cause the eye to make less fluid. Others lower pressure by helping fluid drain from the eye. Glaucoma medicines may be taken several times a day. Since glaucoma often has no symptoms, people may be tempted to stop taking or may forget to take, their medicine. You need to use the drops or pills as long as they help control your eye pressure. Regular use is essential.
- Laser Trabeculoplasty: Laser trabeculoplasty helps fluid drain out of the eye. Your doctor may suggest this step at any time. In many cases, you need to keep taking glaucoma drugs after this procedure. Laser trabeculoplasty is performed in your doctor’s office or eye clinic. Before the surgery, numbing drops will be applied to your eye. As you sit facing the laser machine, your doctor will hold a special lens to your eye. A high-intensity beam of light is aimed at the lens and reflected onto the meshwork inside your eye. You may see flashes of bright green or red light. The laser makes several evenly spaced burns that stretch the drainage holes in the meshwork. It allows the fluid to drain better.
- Glaucoma Filtering Surgery: Conventional surgery makes a new opening for the fluid to leave the eye. Your doctor may suggest this treatment at any time. Conventional surgery often is done after medicines, and laser surgery has failed to control pressure. Before the surgery, you will be given medicine to help you relax. Your doctor will make small injections around the eye to numb it. A small piece of tissue is removed to create a new channel for the fluid to drain from the eye.
As with laser surgery, conventional surgery is performed on one eye at a time. Usually, the operations are four to six weeks apart. Conventional surgery is about 60 to 80 percent effective at lowering eye pressure.
Glaucoma Surgeons in Delhi at Eye7 Chaudhary Eye Centre
Glaucoma FAQ
Not necessarily. Increased eye pressure means you are at risk for glaucoma but does not mean you have the disease. A person has glaucoma only if the optic nerve is damaged. If you have increased eye pressure but no damage to the optic nerve, you do not have glaucoma. However, you are at risk. Follow the advice of your eye care professional.
Not necessarily. Not every person with increased eye pressure will develop glaucoma. Some people can tolerate higher eye pressure better than others. Also, a certain level of eye pressure may be high for one person but normal for another. Whether you develop glaucoma depends on the level of pressure your optic nerve can tolerate without being damaged. This level is different for each person. That’s why a comprehensive dilated eye exam is very important. It can help your eye care professional determine what level of eye pressure is normal for you.
Yes. Glaucoma can develop without increased eye pressure. This form of glaucoma is called low-tension or normal-tension glaucoma. It is not as common as open-angle glaucoma.
- If you have a family history of glaucoma
- If you experience blurring of vision
- If you see haloes around light
- If you suffer from frequent headaches
- Frequent change of glasses due to decreasing eyesight
A glaucoma suspect is a person in who, in the doctor’s opinion, there is a high chance of developing glaucoma. It may be due to the elevated eye pressure or the appearance of the optic nerves. Some people may have pressures that are higher than normal, but is not associated with optic nerve damage and vision loss but they do not develop glaucoma and are called ocular hypertensives. Other people have optic nerves that might appear to be abnormal, but, in fact, are normal for them.
If you are over age 60, diabetic or have a family member with glaucoma, you are at higher risk for glaucoma than others. Risk factors for glaucoma, rest will reach you one by one
If eye drops have been prescribed for treating your glaucoma, you need to use them properly and as instructed by your eye care professional. Proper use of your glaucoma medication can improve the medicine’s effectiveness and reduce your risk of side effects. To correctly apply your eye drops, follow these steps:
- First, wash your hands.
- Hold the bottle upside down.
- Tilt your head back.
- Hold the bottle in one hand and place it as close as possible to the eye.
- With the other hand, pull down your lower eyelid which forms a pocket.
- Place the prescribed number of drops into the lower eyelid pocket. If you are using more than one eye drop, be sure to wait at least five minutes before applying the second eye drop.
- Close your eye or press the lower lid lightly with your finger for at least one minute. Either of these steps keeps the drops in the eye and helps prevent the drops from draining into the tear duct, which can increase your risk of side effects.