LASIK screening is the most important and time-consuming part of the whole process of Laser Vision Correction (Read the detailed steps at https://www.eye7.in/lasik-eye-surgery/). At Eye7 Chaudhary Eye Centre, LASIK screening involves a six-step protocol, before one can be declared fit for LASIK. The screening process may take almost 2 hours whereas the LASIK procedure itself takes just 15 minutes to treat both the eyes.
The screening process includes the following steps:
1: Refraction
Correct refraction is the most important part of Laser correction. A doctor may have the best laser equipment, but if the refraction or determining the correct power of the eye is not accurate, the results of laser correction will naturally be not optimal.
A good refraction includes the following:
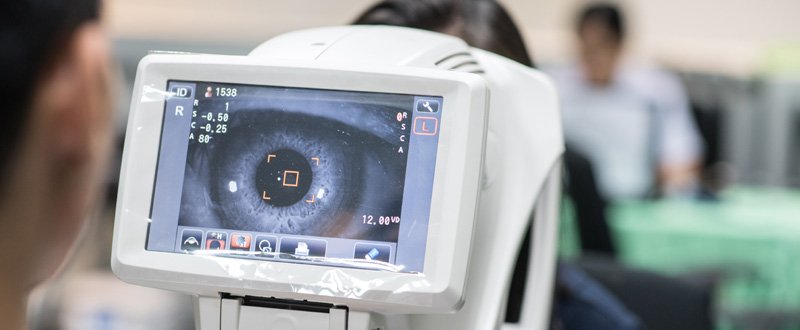
- Auto-refractometer testing: This is also popularly referred to as the Computerized eye testing. The patient is asked to bring his head in front of the machine. The chin is supported on the chin rest. The device is focused on the eye while the patient looks at a target in the body of the machine. On press of a button, the machine determines the refractive error of the eye and the same shows on the computer screen on the machine. Three readings are taken, and the average of the three readings are used as the reference spectacle power of the eye. An auto-refractometer is a fairly accurate measuring device and is taken as a refractive guide. Complete reliability can never be placed on this form of measurement.
- Dilated refraction: This is the most important part of the spectacle power assessment of the eye. Pupil dilating eye drops are instilled in the eye two to three times at an interval of 5 minutes, and the patient asked to close his eyes and wait in the waiting area till the pupil dilates. It may take 20 to 30 minutes.
The optometrist now conducts retinoscopy with a retinoscope to determine the power of the eye. The patient is asked to look at a vision testing screen at a distance of 20 feet (6 meters), while the optometrist checks out the power of the eye with the help of a whole tray of miniature lenses. Dilating the pupils puts the ciliary muscle of the eye to rest, and eliminates errors in determining the true refractive power.
- Post Mydriatic test (PMT): This is also referred to as the dry refraction, or the refraction of the person when the pupils are not in a dilated state. It is also called the true refraction or the final refraction which is used for vision correction. This test is done at least 24 hours after the dilated refraction. In this test, trial lenses are placed in the trial frame mounted in front of the eye. The best vision correction with glasses is determined. The dilated refraction is taken as a guide for this dry refraction. It is usually seen that the dry refraction is about 0.25 more than the dilated refraction. This difference in number is due to the relaxing of the ciliary muscle of the eye due to the mydriatic effect of pupil-dilating drops. NOTE – Though the above protocol is the best way to determine the most accurate refraction, not all situations warrant a dilated refraction. Simple myopia or myopia with small astigmatism may be treated with a laser without a dilated refraction. The eye specialist decides what works best in his hands.
2: Intra Ocular Pressure (IOP) Measurement
The human eyeball is in a shape of a globe. The core of the ball is a cavity which is filled with fluid. Fresh fluid is continuously secreted within the eye, replacing the old fluid which flows out of the eye through drainage channels. The inflow-outflow balance can maintain a certain pressure in the eye to keep it inflated (prevents the eyeball from collapsing). The normal IOP ranges from 12 to 19 mm of Hg.
The Intra Ocular pressure is determined by:
- Non-Contact Tonometer (NCT): This is the Air Puff method. A metered Air Puff is directed on the cornea, and the degree of compression or applanation of the cornea is determined to calculate the pressure of the eye. It is a rapid screening method, with a slightly low-reliability index.
- Applanation Tonometer (AT): This is considered the gold standard in measuring the pressure of the eye. This test is done when the rapid screening test as done by NCT gives a suspicious reading of a high IOP. The test involves calculating the amount of pressure required to applanate (press) a portion of the cornea is read off as the IOP of the eye. Since the applanating device has to be brought in contact with the cornea, numbing eye drops have to be used. This test helps to cross check the readings of the NCT.
- Clinical Importance of IOP: Steroid eye drops are almost always used after LASIK for 1 to 4 weeks during the process of recovery. Some people tend to develop a raised IOP as a result of these drops. This raised pressure is referred to as a Secondary Glaucoma. A raised IOP can damage the optic nerve of the eye if the pressure is allowed to stay high for a long time. Such people who respond to steroid drops are referred to as Steroid Responders. If the normal pre LASIK eye pressure is known, the early rise in pressure can be detected, and suitable remedial measures are taken. These include stopping the steroid drops and adding IOP lowering medicines to the treatment regime. The pressure tends to regain normal values in about 2 to 3 weeks’ time. If properly managed, it is hardly ever associated with any actual loss of vision. The pressure changes as a response to steroid drop usually happen at about a week or two of instillation of these drops. The incidence of Steroid Responders is very low. Still one has to be alert to this situation.
3: The Corneal Scanning and Thickness by Pentacam or Ultrasound
- A normal thickness of an Indian cornea is around 530 microns or 0.53 mm.
- A cornea which is less than 495 microns is considered thin and should be treated with caution.
- A cornea which is less than 450 microns is considered very thin, and LASIK should not be done on such a cornea.
- Corneal scanning evaluates the corneal profile of the entire cornea, end to end. It also determines the ratio of the anterior to the posterior curvature of the cornea. It is useful to pick up early corneal deformities, abnormal thinning or weakness of the cornea. It is best to avoid LASIK if an abnormal pattern is seen.
4: Screening for Any Associated Eye Pathology
- LASIK is only done on healthy eyes.
- If an eye has any associated eye disease like Keratoconus or any other corneal pathology, glaucoma, retinal pathology, etc. resulting in decreased vision, then LASIK should preferably be avoided.
- Systemic diseases like collagen disorders like SLE. Lupus etc. should be considered a contraindication.
5: Retina Evaluation
In myopia, the eye becomes bigger in size. As a result, the retina inside the eye gets stretched. Stretching beyond a certain limit as seen in high myopia can lead to retinal stretch marks called lattice and may be associated with abnormal thinning of the retina in these areas. Such thinned out areas may also develop a hole. Retinal holes are potentially dangerous as at a later time in life they may extend and cause a retinal tear or detachment resulting in partial or permanent loss of vision. It is important to have the retina checked by a retina specialist to rule out these situations. If a dangerous lattice or a hole is seen, it should be lasered by a retina laser to seal it. The tissue response generated by the laser takes 2 to 3 weeks to seal the hole fully. LASIK should be done after the sealing process is complete. In insignificant lattice or holes, LASIK may be done before, and the lesion may be kept in observation or sealed at a later date.
6: Dry Eye Testing
LASIK involves cutting and ablation of the tip of the corneal nerves during the process of laser corneal ablation, and it results in dryness. The nerves regenerate in 3 to 6 months’ time, and the dryness likewise, disappears in 3 to 6 months’ time. During this period, lubricating eye drops have to be given. However, if the eyes are dry from before, the dryness post LASIK may get aggravated, and may require more vigorous lubricant treatment or other alternatives. It is therefore important to do dry eye testing before doing LASIK
- Shirmer’s test is considered a fairly dependable and simple test to access the tear secretions in the eye and determine the grade of dryness. A special filter paper bent at one end, is placed in the eye between the eyeball and the lower lid. After 5 min, the wetting on this strip is seen. If the wetting is 30 mm or more, the tear function is normal. If the wetting is 10 mm or less, this eye may have pre-existing dryness.
- Tear film breakup time test is another test for evaluating dry eyes. Numbing eye drops with a special stain are put in the eye, and the interval between a complete blink and appearance of a first random dry spot on corneal is noted. Its normal values range from 15 to 35 seconds. A value less than 10 seconds is indicative of dry eye.